How GLP-1s change your relationship with food
Wegovy, Ozempic, and Mounjaro change how your body handles hunger. They aren't just about willpower or cutting calories; they mimic the GLP-1 hormone to slow down digestion and tell your brain you're full sooner.
Because of these effects, diet becomes paramount. The old advice of 'eat less, move more' falls short when your body’s signals are being modified. Simply cutting calories can lead to muscle loss and isn’t sustainable long-term. We need to focus on what we eat, not just how much. The goal isn’t deprivation, it's recalibrating your metabolism.
You're likely seeing the term 'GLP-1 friendly' appearing on food labels. This is a relatively new development, with companies responding to the increased demand for foods that support these medications. While helpful, remember this is still a developing area, and those labels aren’t standardized. It's about understanding the principles of what makes a diet supportive of GLP-1 action, and not just relying on marketing. This is a metabolic shift, and it requires a thoughtful, personalized approach.
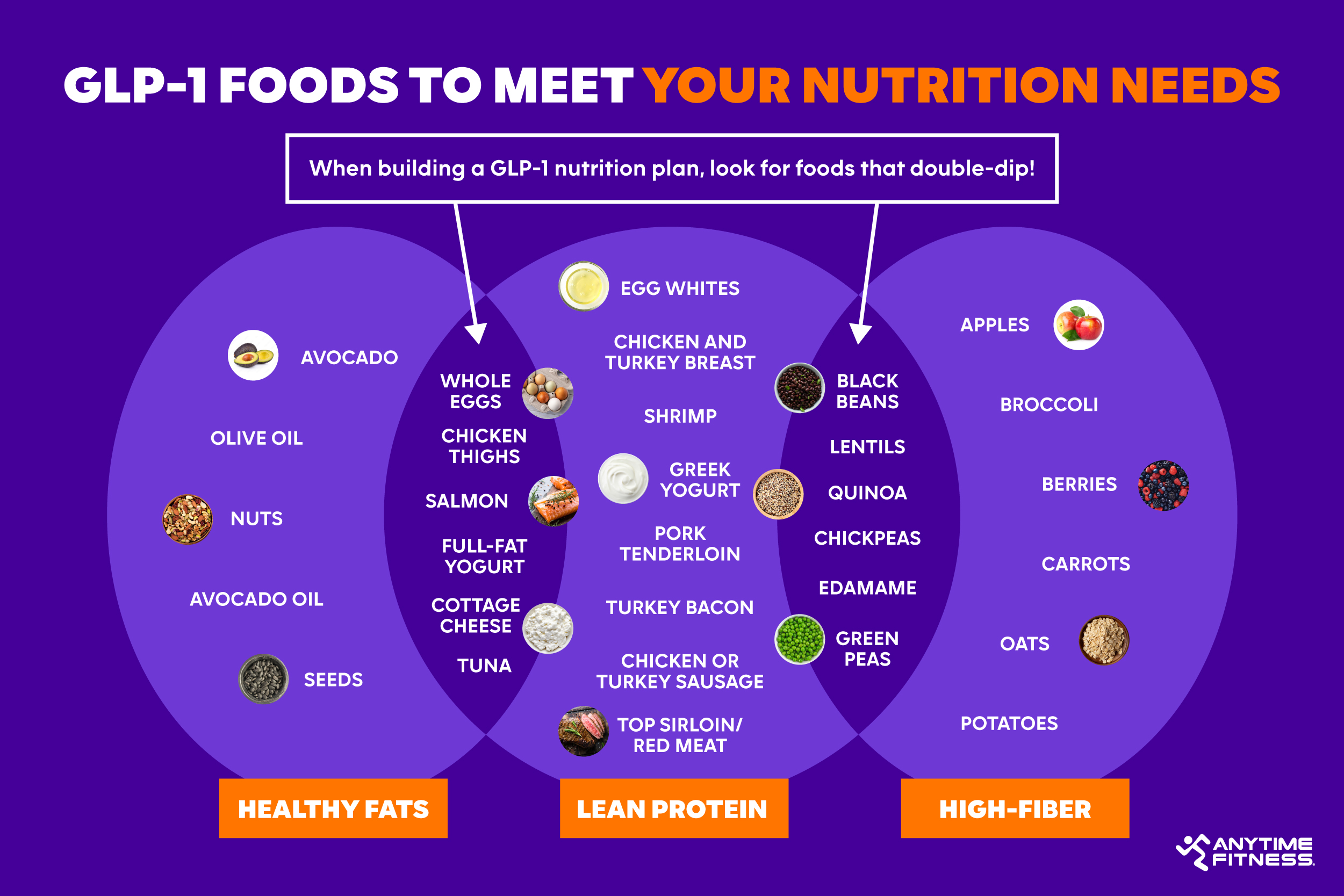
Eat enough protein to protect your muscle
Protein is absolutely essential when using GLP-1 medications. These drugs can cause weight loss, and we want to ensure that loss is primarily fat, not valuable muscle mass. Adequate protein intake helps preserve lean tissue, which is vital for maintaining metabolism and overall health.
Aim for consistent protein intake throughout the day. A general guideline is around 0.8 to 1.2 grams of protein per kilogram of body weight, but this can vary. Excellent sources include lean meats like chicken and turkey, fish (salmon, tuna), legumes (beans, lentils), tofu, and Greek yogurt. Consider portion sizes – a palm-sized serving of protein is a good starting point.
Nausea is common. If you're struggling to keep food down, stop trying to eat three big meals. Small snacks like a few bites of chicken or a bit of yogurt throughout the day are easier on the stomach than one heavy dinner.
Fiber helps with more than just digestion
Fiber isn’t just about keeping things "regular" – it plays a critical role in optimizing the effects of GLP-1 medications. Both soluble and insoluble fiber contribute to gut health, but soluble fiber is particularly beneficial. It slows down digestion, promotes a feeling of fullness, and can help regulate blood sugar levels.
Excellent sources of fiber include beans and lentils, oats, berries, broccoli, and whole grains like quinoa and brown rice. Aim for at least 25-35 grams of fiber per day. However, increasing fiber intake too quickly can cause gas and bloating. Start slowly and gradually increase the amount over several weeks.
Pay attention to how your body responds. Some people find they need to adjust their fiber intake based on their individual tolerance and the specific GLP-1 medication they're using. A diverse gut microbiome, supported by fiber, is a key component of long-term metabolic health.
- Soluble Fiber: Dissolves in water, forming a gel-like substance. Found in oats, beans, apples, and citrus fruits.
- Insoluble Fiber: Doesn't dissolve in water. Adds bulk to stool. Found in whole wheat bread, vegetables, and wheat bran.
Soluble vs. Insoluble Fiber: Impact on GLP-1 Diet & Digestion
| Fiber Type | Primary Sources | Impact on Digestion | Impact on Blood Sugar | Potential Side Effects (Especially with GLP-1 Agonists) |
|---|---|---|---|---|
| Soluble Fiber | Oats, beans, apples, citrus fruits, psyllium | Dissolves in water to form a gel-like substance; slows down digestion. | Helps regulate blood sugar levels by slowing glucose absorption. | May cause bloating or gas, especially when intake is increased rapidly. Potential for increased fullness, which can exacerbate GLP-1 induced nausea if not managed. |
| Insoluble Fiber | Whole wheat bread, vegetables (like broccoli and carrots), wheat bran | Adds bulk to the stool and promotes regularity; speeds up the movement of food through the digestive system. | Has a minimal direct impact on blood sugar levels. | Generally well-tolerated, but excessive intake can contribute to constipation. May worsen existing digestive discomfort when combined with GLP-1 medication. |
| Soluble Fiber - Fermentation | Certain fruits, vegetables, and oats | Fermented by gut bacteria, producing short-chain fatty acids (SCFAs) which have various health benefits. | SCFAs may improve insulin sensitivity. | Gas and bloating are common due to fermentation. Individuals on GLP-1 agonists should monitor tolerance. |
| Insoluble Fiber - Bulk Forming | Vegetable skins, whole grains | Increases stool volume and promotes bowel movements. | Minimal impact on blood sugar. | Can contribute to feelings of fullness, and in some cases, may exacerbate constipation if not adequately hydrated. Monitor closely while on GLP-1 medication. |
| Combined Fiber Intake | A balanced diet rich in fruits, vegetables, and whole grains | Provides a synergistic effect, promoting both regularity and blood sugar control. | Optimizes blood sugar management and supports overall metabolic health. | Potential for digestive upset (bloating, gas, constipation) is present; gradual increases in intake and adequate hydration are crucial, especially when using GLP-1 agonists. |
| Fiber & GLP-1 Considerations | All fiber sources | GLP-1 agonists slow gastric emptying; fiber further contributes to this effect. | Fiber can help stabilize blood sugar, complementing the action of GLP-1 agonists. | Increased risk of nausea, bloating, and constipation. Careful monitoring of tolerance and adjustments to fiber intake are essential. |
Illustrative comparison based on the article research brief. Verify current pricing, limits, and product details in the official docs before relying on it.
Fat: Quality Over Quantity
Healthy fats are important for satiety, hormone production, and overall health, even when using GLP-1s. However, the type of fat you consume is far more important than the total amount. Focus on unsaturated fats like those found in olive oil, avocados, nuts, and seeds.
I'm not sure there is a perfect fat ratio that works for everyone. While 20% to 30% of calories is a standard starting point, you should see how you feel. Some people find that too much fat while on these meds leads to immediate indigestion.
It’s possible that GLP-1s could slightly impact fat absorption. While this isn’t a major concern for most people, it’s something to be aware of. Prioritizing high-quality fats ensures you’re getting the most nutritional benefit.
Carbohydrate Choices: Timing and Type
Stick to complex carbs like oats, berries, and beans. White bread and sugary drinks cause blood sugar spikes that can make the medication's side effects feel worse. You want the slow-burning energy that comes with high-fiber foods.
Consider carbohydrate timing. Pairing carbohydrates with protein and healthy fats slows down absorption and helps prevent blood sugar spikes. For example, instead of eating a piece of fruit on its own, pair it with a handful of nuts or a serving of Greek yogurt.
Some people find they need to reduce their overall carbohydrate intake while on GLP-1s. This isn’t necessarily required, but it’s something to consider if you’re struggling to manage your weight or blood sugar levels. Experiment to find the carbohydrate intake that supports your individual goals.
Don't ignore hydration and electrolytes
Staying hydrated is crucial, especially when using GLP-1 medications. These drugs can sometimes cause nausea, vomiting, or altered digestion, which can lead to dehydration. Aim to drink plenty of water throughout the day.
Don’t forget about electrolytes – sodium, potassium, and magnesium. These minerals are lost through sweat and can be further depleted if you’re experiencing diarrhea or vomiting. Incorporate electrolyte-rich foods like bananas, spinach, and avocados into your diet, or consider an electrolyte drink.
- Drink water consistently throughout the day.
- Include electrolyte-rich foods in your meals.
- Consider an electrolyte drink if you're experiencing dehydration symptoms.
Food Combinations for Optimal Results
Putting it all together, here are some meal and snack ideas that combine the principles we’ve discussed. Remember, these are suggestions – experiment to find what works best for you and your individual preferences.
Breakfast: Greek yogurt with berries and a handful of almonds. This provides protein, fiber, and healthy fats to start your day. Lunch: Salmon with roasted vegetables (broccoli, Brussels sprouts) and a side of quinoa. This offers lean protein, fiber, and complex carbohydrates. Dinner: Chicken salad (made with Greek yogurt instead of mayonnaise) with whole-grain crackers and avocado. This provides protein, healthy fats, and fiber.
Snacks: A hard-boiled egg with a small apple. A handful of nuts and seeds. Cottage cheese with a few berries. Be mindful of portion sizes. Even healthy foods can contribute to weight gain if eaten in excess. The goal is to create balanced meals and snacks that keep you feeling full and satisfied.
Navigating GI Side Effects with Food
Common gastrointestinal side effects like nausea, constipation, and diarrhea are possible with GLP-1 medications. Dietary adjustments can often help manage these symptoms. If you’re experiencing nausea, opt for bland foods like toast, crackers, and rice. Smaller, more frequent meals can also be easier to tolerate.
Constipation can be addressed by increasing your fiber intake (gradually!) and staying well-hydrated. Diarrhea might require reducing fiber intake temporarily and avoiding trigger foods like dairy or caffeine. Identifying your personal trigger foods is key.
If side effects are severe or persistent, it's important to talk to your doctor. They can help determine if the medication needs to be adjusted or if there are other underlying issues. It's okay to adjust your diet to find what works for you, and remember that discomfort is sometimes a part of the process. Don’t suffer in silence – seek guidance when needed.
- For nausea: Try bland foods like crackers or white rice and eat slowly.
- For Constipation: Increase fiber gradually, drink plenty of water.
- For Diarrhea: Reduce fiber, identify trigger foods, stay hydrated.





No comments yet. Be the first to share your thoughts!